Medicaid Programs Nationwide Drop Coverage of Weight Loss Drugs
Thirteen states now cover expensive GLP-1 weight loss drugs through Medicaid, down from 16 last year as budget pressures force coverage cuts.
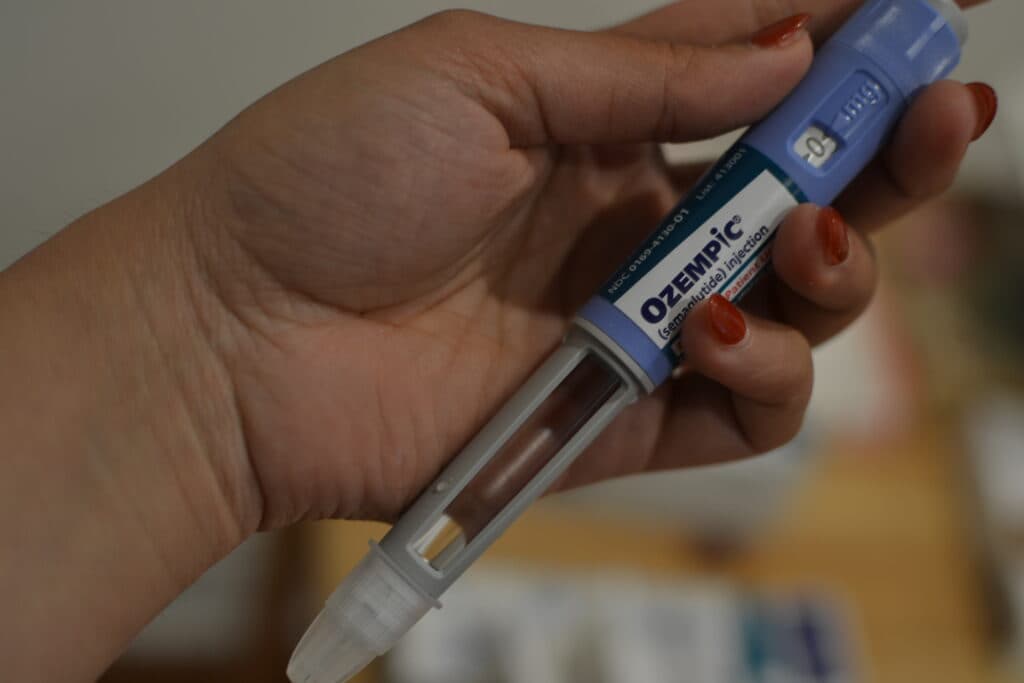
COLUMBUS, OHIO — More states are removing coverage for expensive GLP-1 weight loss medications from their Medicaid programs as budget concerns mount, with Massachusetts and Rhode Island now considering joining the list of states that have discontinued the costly treatment.
Thirteen state Medicaid programs currently cover GLP-1 drugs for obesity treatment this year, down from 16 last year, according to health policy research group KFF. The medications, which include popular brands like Ozempic, have proven effective for weight loss but carry substantial costs that strain state budgets.
California, New Hampshire, Pennsylvania and South Carolina have already eliminated coverage of the drugs for weight loss due to financial pressures on their Medicaid programs. The trend reflects the challenging balance states face between providing comprehensive healthcare coverage and managing limited resources.
Budget Proposals Target Coverage
In Massachusetts, the governor’s proposed fiscal 2028 budget would remove funding for the state’s Medicaid program, MassHealth, to cover GLP-1 medications for weight loss alone. The state would continue covering the drugs for diabetes and other medical conditions, though the legislature is still debating the budget proposal.
Rhode Island’s governor has similarly proposed removing GLP-1 coverage from the state’s Medicaid program specifically for weight loss treatment. The proposal represents another potential reduction in access to the medications for low-income patients.
State-by-State Coverage Varies
Among states that continue providing coverage, Medicaid programs in Delaware, Kansas, Michigan, Minnesota, Mississippi, Missouri, Tennessee, Utah, Virginia and Wisconsin still cover the drugs for obesity treatment, according to KFF data.
However, some states have implemented restrictions to control costs. Michigan has limited eligibility for these medications to patients with morbid obesity rather than those who are overweight or obese. The move is expected to save the state an estimated $240 million.
North Carolina provides an example of the ongoing policy debates surrounding these medications. The state reinstated coverage in mid-December after having dropped it in October, demonstrating the fluid nature of coverage decisions as states wrestle with budget constraints.
The coverage reductions come as healthcare advocates emphasize the potential long-term health benefits and cost savings that effective obesity treatments could provide. However, the immediate budget impact of covering the expensive medications has proven challenging for state Medicaid programs operating under tight fiscal constraints.